DENTAL HISTORY
Deadly disease discovered
A CDC report identifies a new disease with an alarming mortality rate. However, no safety protocols were established to deal with the new HIV epidemic.
 1981
1981
No regulations
An HIV-positive dentist in Florida continued to practice, highlighting a glaring issue: there were no regulations in place for infected dental practitioners. Consequently, practitioners could continue working with concealed illnesses. Moreover, there were no regulations governing the disclosure of inherent risks associated with certain dentists to the public.
 1987
1987
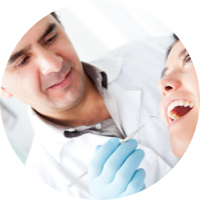
First dentist-to-patient transmission of HIV
CDC report announces first dentist-to-patient transmission of HIV in a clinical setting. Kimberly Bergalis, age 23, died after contracting the HIV virus from dentist Dr. David J. Acer. The Bergalis case established a public outcry for public reforms in regards to the way patients were treated and how healthcare professionals should have to inform patients if they were infected. This case also sparked the need to make drastic reforms on how infection control protocols and safety equipment should be used in a medical setting.
 1991
1991
Protective equipment becomes mandatory
Personal protective equipment (gloves, masks), and barrier equipment becomes mandatory for dentists. It is important to note that eleven years lapsed between this groundbreaking rule change and the very first AIDS case identified in San Francisco by the CDC in 1981. It took eleven years for the healthcare industry to realize gloves and masks should be mandatory operating procedure. The Dr. Acer dental scare was the only reported case during this time period. How many other cases do you think went unreported in those eleven years?
 1992
1992
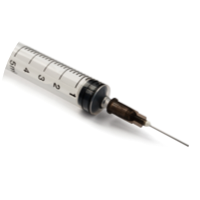
No more boiling needles
Science proved that the practice of boiling needles in water was not an effective sterilization method. Reusing of needles was also banned due to lack of proper sterilization processes.
 Exact Date Unknown
Exact Date Unknown
First case of patient-to-patient transmission of hepatitis C
Dr. Scott Harrington's office in Oklahoma is the first case of patient-to-patient transmission of hepatitis C in a clinical setting. Due to lack of proper infection control protocols, over 7,000 patients were informed to seek medical blood testing to test for HIV, hepatitis B and C. Of the patients tested, 89 tested positive for hepatitis C, 5 for hepatitis B, and 4 for HIV. 2013
2013
SAFETY BREACHES ARE A PART OF DENTAL HISTORY
Scientific and technological advances have helped to create safer dental treatments; however, we still have a long way to go to ensure patients are truly safe at a dental office. A major problem is that there are still devices being used in dental offices, the safety of which we now know to be questionable. Until the public becomes aware of the inherent safety risks these devices pose, dentistry will continue to use them.
State-mandated health inspections only occur when a whistleblower or patient voices their concerns. Consequently, dentists, orthodontists, and hygienists are often left on their own to ensure they are following all health and safety protocols. Nevertheless, safety breaches remain a constant issue at dental offices. Globally, there are cases of gross negligence involving dentists, orthodontists, and hygienists taking shortcuts, which can have a significant impact on you and your family. Therefore, it's crucial to learn from past mistakes; otherwise, we are doomed to repeat them.
What will it take to make the necessary changes? Could it possibly require you or your family getting sick to spark change? Instead of relying on retroactive steps, we must proactively take preventive measures.
To learn more about how serious these issues are please click on the links below.


